By Joe Alton, M.D.
If confronted by a fast-moving wildfire, your chances of avoiding death or injury depend on a plan of action that is easy to understand and quick to implement. Some form of communication system should be established with your loved ones that would function even in dire situations. Texting on your cell phone, for example, requires less bandwidth than voice calls so is more likely to get through during an emergency.
If you must flee via car, have a bag already packed with food, water, extra clothes, batteries, flashlights, and a first aid kit. These are standard items in any “grab ‘n’ go” bag and every family should have one ready for any emergency. Make sure you make allowances for children, pets, and those with chronic medical issues; have medications and supplies geared for their needs.
If your routes of vehicular escape are blocked and you are forced to escape by foot, make sure you’re dressed in long pants, sleeves, and heavy boots. A wool blanket is very helpful as an additional outside layer because the material is relatively fire-resistant. Some people think it’s a good idea to wet the blanket first: Don’t. Wet materials transfer heat much faster than dry materials and will cause more severe burns.
Don’t forget to bring your cell phone, any important documents you might need, and some cash in small bills. If the electricity is out, credit card processing may not be an option and you’ll lose a different but very important type of power: purchasing power.
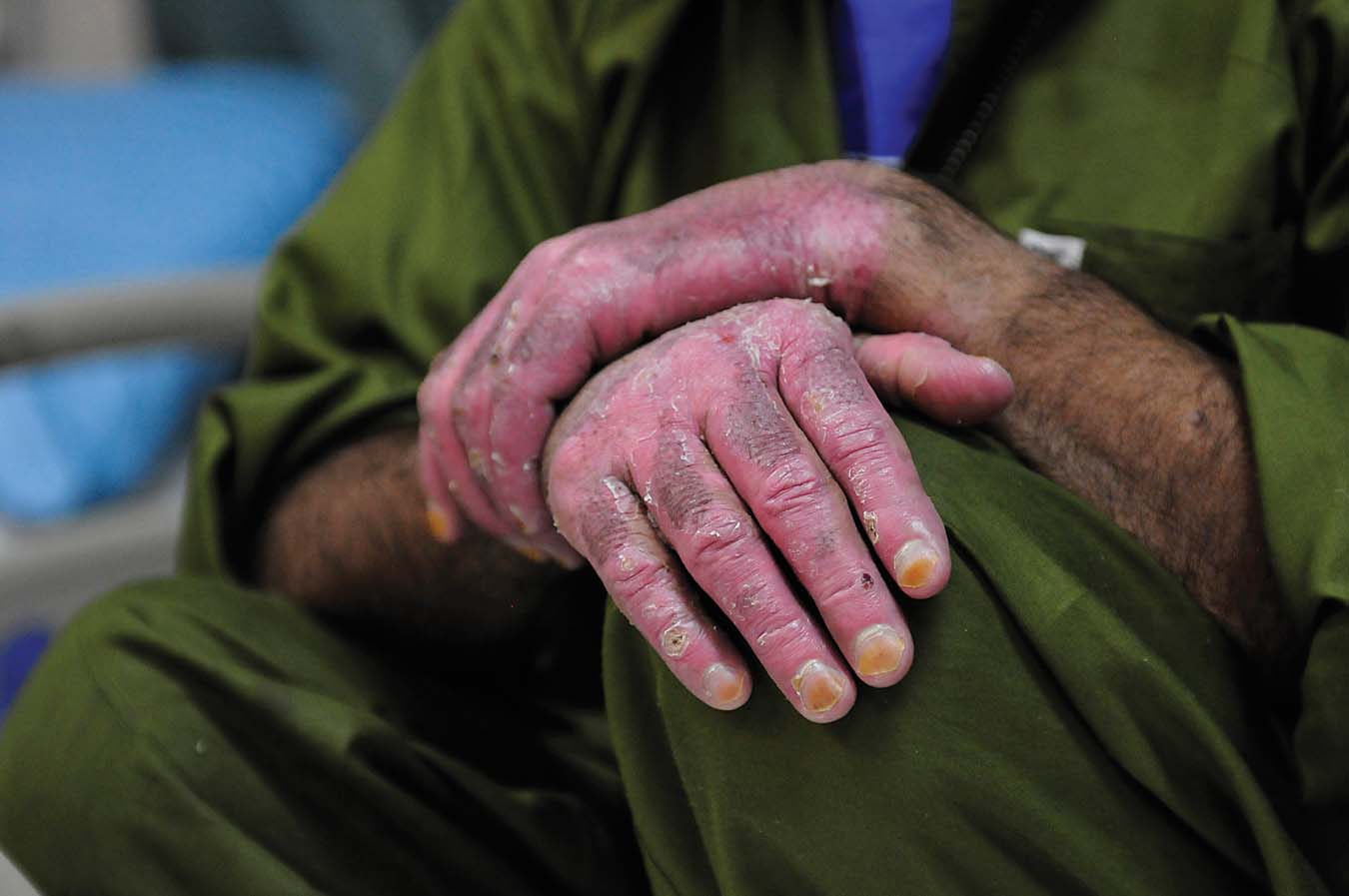
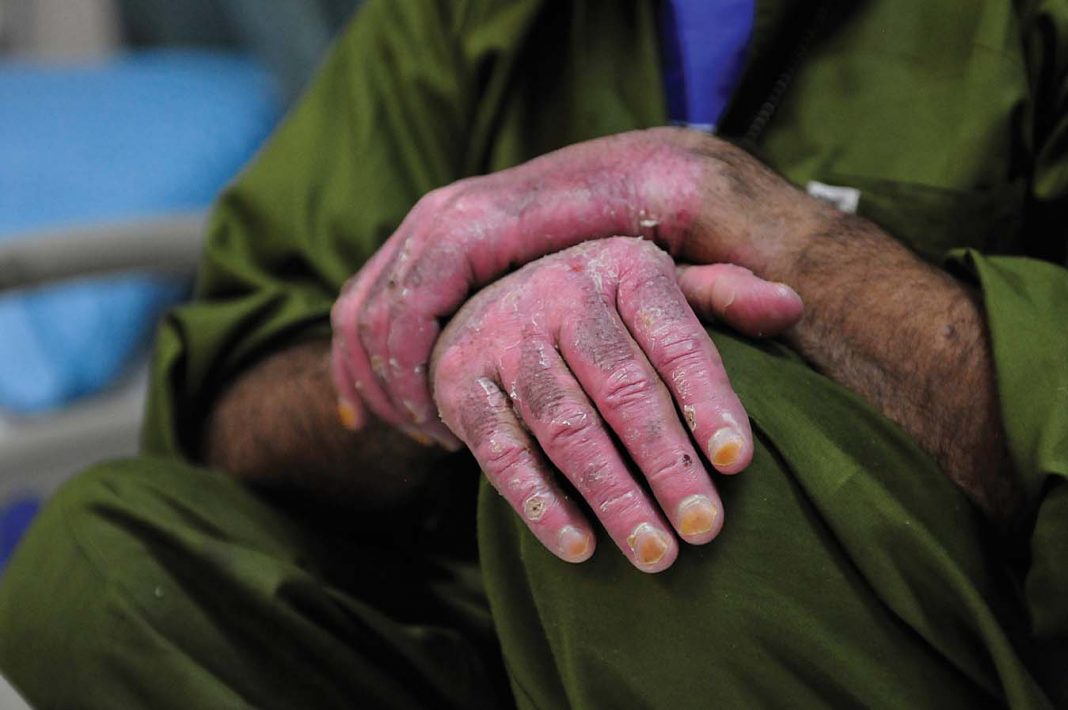
Treating burns can be difficult, and healing can be slow and painful.
Medical kit items especially useful in wildfires include face masks, eye gear that protects from smoke, work gloves to protect hands, burn ointment, and non-stick dressings. N95 face masks are preferred as they provide a tight facial fit and filter out 95% of particles greater than 0.3 microns in size.
You may see “wildfire medical kits” online, but the differences from any standard medical kit are usually more face masks and burn gel, a “HELP” sign, and a whistle to notify others that you’re in need of aid. If you have the time and inclination, consider putting together your own quality kit. For example, signs may not be visible in smoky areas, so a powerful flashlight is a good item to have on hand. As a signal, the reflection from a compact mylar (solar) blanket (4 ½ by 7 feet in size when unfolded) would be more noticeable, especially from a distance.
Specialized burn dressings are available commercially but can also be improvised with gauze pads and petroleum jelly or aloe vera. Rolls of gauze and medical tape can be used for additional coverage. Other items that will come in handy are scissors, cold packs, wool blankets, and some eyewash (smoke is a major irritant to the eyes).
Trapped in a building
The wisest course of action is to leave before your home is in imminent danger of being engulfed by the wildfire. If you have no choice but to stay inside the building, retreat to the side farthest from the fire and with the least number of windows, as windows transfer heat to the inside. Stay there unless you have to leave due to smoke or the building catching fire.
If that’s the case, wrap yourself in the wool blanket, leaving only your eyes uncovered. If smoke is making it difficult to breathe, get as low as you can and crawl out of the building. There’s less smoke and heat the lower you go. Touch doorknobs and spaces around doors with the back of your hand before trying to open them. If the door is very warm, it’s best to try another escape route.
Always keep your face down towards the floor to protect your airway. You can recover from burns on your skin, but not from significant burns in your lungs.
Smoke inhalation
According to the National Fire Protection Association (NFPA), most people who die in wildfires aren’t burned to death; they succumb to smoke inhalation.
Common causes of smoke inhalation include:
Simple combustion: Combustion uses up oxygen near a fire; the deficit of this vital element can kill a person outright. The larger the fire, the more oxygen it removes from the area.
Carbon dioxide: Some by-products of smoke may not directly kill a person, but could take up the space in the lungs that oxygen would ordinarily occupy. Even the expulsion of a large bubble of carbon dioxide can kill wildlife near it, such as in the example of “swamp gas.”
Chemical irritants: Many chemicals found in smoke can cause injury when they come in contact with lung tissue. This amounts to an internal burn which causes swelling and airway obstruction. Chlorine gas used in World War I is an example of a deadly chemical irritant.
Other asphyxiants: Carbon Monoxide (most common), cyanide, and some sulfides may interfere with the body’s ability to utilize oxygen.
Symptoms may include:
- Cough
- Shortness of breath
- Hoarseness
- Upper airway spasm
- Eye irritation
- Headaches
- Pale, bluish or even bright red skin
- Loss of consciousness leading to coma or death
A patient with smoke inhalation may present with soot in the throat and nasal passages. Both of these areas may be swollen and irritated.
Once you suspect that a wildfire victim suffers from smoke inhalation, move them immediately to an environment where there is clean air or, at least, portable oxygen. Be very careful not to put yourself in a situation where you are likely to succumb to smoke inhalation yourself. A mask, hand, and eye protection should be worn before attempting a rescue. Be prepared to begin CPR if necessary.
Don’t expect a rapid recovery from significant smoke inhalation. The victim will experience shortness of breath with the slightest activity and be very hoarse. These symptoms may go away with time, but permanent disability is possible.
Burns
Of course, anyone who sustains a serious burn should be transported immediately to a hospital, preferably one with a dedicated burn unit. In the midst of a wildfire, however, these facilities may be inaccessible or overwhelmed by a large number of casualties. Therefore, the average citizen may be required to provide burn care in disaster settings.
The percentage of body surface area is often used to determine the severity of injury. A system known as the “rule of 9’s” is thought to give a rough estimate of potential risks. Off or on the grid, burns may best be categorized by “degrees,” a measure related to the depth of penetration. The deeper the burn damage, the graver the consequences for the victim.
First-degree burns: First-degree burns affect the epidermis, the topmost layer of the skin. A typical example would be a “sunburn.” These burns appear red, warm, and dry, and are painful to the touch. Mild swelling may occur. Dry, dead skin will cause itching as it eventually peels off. No scarring is expected.
Treatment for a first-degree burn includes:
- Cool water soaks for five to ten minutes (many make the mistake of running cold water over the burned area for only a few seconds). Avoid ice, which traumatizes already-damaged skin by decreasing circulation to it.
- Pain relievers like ibuprofen (Advil) or acetaminophen (Tylenol). After a day or so, the pain will subside.
- Anesthetic ointments and burn gels containing aloe vera.
- Antihistamines for itching.
Expect complete healing in a week or so.
Second-degree burns: Second-degree burns, sometimes called “partial-thickness” burns, affect the deep layer of the skin (the “dermis”). You will see areas that are painful, swollen, and appear moist rather than dry. The area will have a tendency to weep clear or whitish fluid. These injuries often have a number of blisters of various sizes.
Treating a second-degree burn: Treatment for a second-degree burn should be quick and intensive. The faster treatment is begun, the faster the recovery. Consider:
- Running cool water on the burn for 15 minutes or longer.
- Quick removal of rings, bracelets, and necklaces to prevent issues due to rapid swelling.
- Bandaging the wound with non-stick dressings like Telfa pads. Avoid the use of cotton balls as dressings due to the sloughing off of fibers that can increase the likelihood of infection.
- Using specialized burn dressings like Xeroform; similar dressings can be improvised using gauze and petroleum jelly.
- Giving pain medicines as needed.
- Applying antibiotic cream to blisters to prevent infection.
Blisters may be numerous, but should be broken only if very large or it is clear they would break during normal activity or in bed. The “popping” of blisters may increase the risk of infection. If you feel it’s necessary, puncture with a sterilized needle at the base and leave the skin covering the raw area.
Keeping the area protected from infectious organisms is important; dressings should be changed at least daily. Most second-degree burns heal in 2-3 weeks without thick scars, but may leave the skin darker than its original color.
Honey has been used as a coating for significant burns when conventional products are unavailable. Spread it over the wound and cover with plastic wrap. Take care not to apply the plastic completely around an extremity, as subsequent swelling can cause painful compression. A number of other home remedies include vinegar, witch hazel, black tea bags, baking soda, and various herbs.
Third-degree burns: A severe type of burn injury, third-degree burns damage the full thickness of the skin and, often, deeper structures like the nerves and blood vessels below the skin. Once the damage goes through the skin, you have lost your body’s “armor,” causing the rapid loss of fluids and ensuing dehydration. Loss of body heat and infection are also common consequences of this type of burn.
Third-degree burns can vary in appearance based upon the type of burn incurred. They may appear white and waxy, charred brown, or black. The area may feel stiff or “leathery.”
Treating a third-degree burn: As long as the victim’s clothing is not smoldering, don’t remove clothing over the burn. Elevate the burn injury about the level of the heart. Otherwise, follow the steps for a second-degree burn.
Protective coverings for severe burns include products like “Second Skin.” Also, Celox hemostatic gauze, although primarily used to stop bleeding, forms a reasonable gel-like dressing when moistened. Silver Sulfadiazine (Silvadene) cream is helpful in preventing infections in third degree burns.
Long-term care is much more complex, however. The skin lost in a third-degree burn is normally replaced by new skin cells produced by the dermis. The dermis, however, has been destroyed, so skin can only grow from the edges of the wound. This not only takes more time than the patient has, but also results in thick scarring which may affect range of motion. These are known as “contractures.”
A person with third-degree burns over any significant percentage of the body will likely be in shock. Cover the victim with a light sheet or blanket to help preserve body core temperature. In any case, the risk of death is significant and recovery is almost always slow and painful.
Common mistakes when treating burns
Many burns heal without consequence, but certain missteps on the part of the caregiver can complicate the situation:
- Failing to run cool water on the burn for the time recommended.
- Using ice on burnt skin.
- Ignoring airway burns. With smoke inhalation, airways may swell rapidly and cause breathing difficulties. Signs include severe coughing, hoarseness, black-specked sputum, and facial burns.
- Popping blisters unnecessarily. Intervene only when they are very large or interfere with function.
- Assuming a burn is less of an issue than it is. Even a first-degree burn, like an extensive sunburn, can be dangerous if steps aren’t taken to avoid further exposure and keep up the level of hydration.
- Using lard or butter as a home remedy. These substances can trap heat in and cause a delay in healing. Other home remedies, like aloe vera, are preferable.
Joe and Amy Alton are the authors of the #1 Amazon Bestseller and 2017 Book Excellence Award winner in medicine “The Survival Medicine Handbook”. For more articles on medical preparedness, go to their website at www.doomandbloom.net.